While remedial massage tends to focus exclusively on manipulative massage techniques, myotherapy extends beyond massage to offer a broader scope of therapy used to treat complex muscle and musculoskeletal conditions, which remedial massage cannot fix alone. Myotherapy is an evidence-based extension of remedial massage, incorporating a deeper understanding of human anatomy and physiology.
Myotherapy focuses more on acute and chronic musculoskeletal pain and disorders. It can be used to treat conditions such as myofascial pain, lower back pain, tension headaches and migraines, sports injuries (e.g. muscle sprains and tears), tendon pain degenerative pain, and rehabilitation from surgery. Myotherapy also focuses on advanced injury prevention – a Myotherapist can identify a problem before any symptoms show (proactive myotherapy), in order to save potentially expensive treatment costs going forward.
A Myotherapist can provide comprehensive health and fitness advice, including exercises that can improve your physical and mental health.
In Myotherapy we use a variety of modalities to treat our clients. These include massage techniques, dry needling, cupping, electrotherapy, mobilisation, muscle energy techniques, and exercise prescription (may include strengthening, lengthening and mobility).
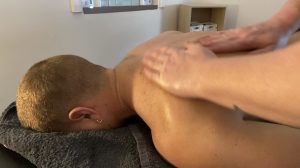
Dry needling is a treatment technique whereby a sterile, single use, fine filament needle is inserted into the muscle to assist with decreasing pain and improving function through the release of myofascial trigger points (knots in muscle).
When the delicate filament needle inserts into the centre of a myofascial trigger point, blood pools around the needle triggering the contracted muscle fibres to relax. It also helps to provide those fibres with fresh oxygen and nutrients, as well as by flushing away any additional acidic chemicals. This reaction, in turn, leads to the decompression of the local blood and nerve supply.
Dry needling can assist in treatment to help release myofascial trigger points (muscle knots), to assist with pain management, and, to restore movement at a joint if inhibited by myofascial trigger points.

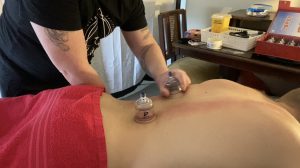
Functional Release Cupping utilises the theories of myofascial cupping, fascial slings, and functional movement patterns to make dramatic changes in range of motion, functional capacity and pain.
This dynamic approach to cupping is highly individualised to the client’s own movement deficits and has been developed with a sound basis in fascial research, clinical reasoning and application in the clinic setting.
FRC takes the traditional concept of myofascial cupping and incorporates an evidence based approach to its application, while ensuring the treatment is highly outcome focused
Joint mobilisation is the application of passive or active assisted rhythmic joint movements using physiological or accessory movements for therapeutic outcomes e.g. pain reduction and / or restoration of optimal joint movement.
Physiological movements (osteokinematic movement): Observable active measurable joint movements e.g. those occurring in the cardinal planes of motion, sagittal, frontal and transverse planes.
Accessory movements (arthrokinematic movement): unobservable movement between adjacent joint surfaces – roll, glide and spin. These movements cannot occur independently or voluntarily and if limited can restrict full pain free physiological motion to take place.
Mobilisation is particularly useful to the myotherapist, as it allows treatment of deep, short, soft tissue structures (ligament, capsule and uni-segmental muscle).
Mobilisation/articulation can be more appropriate when manipulation is contraindicated or not tolerated or preferred by the client/patient.
Joint mobilisation can be performed manually or belt-assisted.
Muscle energy techniques (MET) are a type of manual therapy used by physical therapists and other healthcare professionals to improve joint mobility, increase muscle flexibility, and reduce pain. MET involves using the patient’s own muscle contractions to help lengthen or strengthen muscles and improve joint function.
There are several different types of MET, including post-isometric relaxation (PIR), reciprocal inhibition (RI), and resisted isometric contraction. PIR involves a patient contracting a muscle and then relaxing it to help lengthen a tight muscle. RI involves contracting one muscle group to inhibit the contraction of an opposing muscle group, which can help to increase joint range of motion. Resisted isometric contraction involves contracting a muscle while simultaneously applying resistance, which can help to increase muscle strength and improve joint stability.
MET is often used in conjunction with other manual therapy techniques, such as massage and joint mobilisation, as part of a comprehensive treatment plan. It can be effective for treating a variety of musculoskeletal conditions, such as low back pain, neck pain, and joint dysfunction. MET is generally considered safe when performed by a qualified healthcare professional with expertise in manual therapy.
It is important to note that MET should only be performed by a qualified healthcare professional with training in manual therapy techniques. MET should not be performed on individuals with certain medical conditions, such as acute injuries or fractures, without proper evaluation and medical clearance.
Electrotherapy is a form of medical treatment that uses electrical energy to alleviate pain, promote healing, and improve physical functioning. It involves the application of electrical currents to specific areas of the body through electrodes placed on the skin.
There are many different types of electrotherapy, including transcutaneous electrical nerve stimulation (TENS), interferential current (IFC) therapy, and electrical muscle stimulation (EMS).
TENS is commonly used for pain relief and works by stimulating the nerves that transmit pain signals to the brain, which can help to reduce the sensation of pain. IFC is used for pain relief and muscle stimulation and involves the use of two or more electrical currents that interact with each other to create a larger, deeper current that can penetrate the affected tissues. EMS is used for muscle strengthening and rehabilitation and involves the use of electrical currents to cause muscle contractions.
Electrotherapy is used in a variety of settings, including physical therapy, sports medicine, and pain management clinics. It can be an effective treatment for a range of conditions, including chronic pain, muscle weakness, joint pain, and inflammation, among others. However, as with any medical treatment, electrotherapy should only be used under the guidance of a qualified healthcare professional.
Clinical taping, also known as kinesiology taping or therapeutic taping, is a technique that involves applying a special type of tape to the skin to provide support and facilitate healing. This type of tape is made of a thin, stretchy fabric that is designed to mimic the properties of human skin, allowing for a full range of motion while still providing support.
The tape is applied in specific patterns to target specific muscles or joints, depending on the individual’s needs. The tape works by lifting the skin, which helps to improve blood and lymphatic flow to the affected area, reducing pain and inflammation, and improving muscle and joint function.
Clinical taping is commonly used in physical therapy and sports medicine to help treat a variety of conditions, such as musculoskeletal injuries, postural imbalances, and joint instability. It can also be used to help manage chronic conditions, such as arthritis or fibromyalgia.
The application of clinical tape is generally safe and non-invasive, although it should only be applied by a qualified healthcare professional with training and expertise in the technique. It is important to note that clinical taping should not be used as a standalone treatment, but rather as part of a comprehensive treatment plan that may also include exercise, manual therapy, and other interventions.
Exercise prescription and rehabilitation are two important components of physical therapy and sports medicine that are used to help individuals recover from injury or illness, improve their physical function and mobility, and prevent future injuries.
Exercise prescription involves designing and implementing an individualized exercise program for a specific individual, based on their unique needs and goals. This may involve a combination of cardiovascular, strength, and flexibility exercises, as well as balance and coordination training. The exercise program is tailored to the individual’s physical abilities, medical history, and fitness level, and is designed to be safe and effective.
Rehabilitation is the process of restoring function, reducing pain, and improving physical performance after an injury or illness. It involves a comprehensive approach to care that includes various interventions such as exercise, manual therapy, and other techniques designed to improve range of motion, flexibility, strength, and endurance. The goal of rehabilitation is to help individuals regain as much function and independence as possible and to minimize the risk of future injury or complications.
Exercise prescription and rehabilitation often go hand in hand, as exercise is a key component of the rehabilitation process. Physical therapists and other healthcare professionals work with patients to develop individualized exercise programs that are appropriate for their specific condition and stage of recovery. The program is designed to gradually increase in intensity and duration as the patient progresses through the rehabilitation process, with the ultimate goal of returning to normal function.
It is important to note that exercise prescription and rehabilitation should only be undertaken under the guidance of a qualified healthcare professional with expertise in these areas. They will be able to design a safe and effective exercise program tailored to the individual’s specific needs and monitor their progress to ensure optimal results.